
“Well, that didn’t go as expected.” <– Me, 348,487 times since becoming a mom. The first time I went into labor, I planned to touch up my makeup just after delivery for beautiful mama/newborn photos. In reality, I forgot I was sporting a Breathe Right strip while my husband snapped pics. So glamorous.
That said, I’d never consider (or recommend) going into labor without a birth plan.
Why a Birth Plan?
- Creating a plan gives you a chance to research and decide how you feel about different options ahead of time. Do you want the freedom to eat and sip on labor aid while you birth your baby? What about pain management and skin-to-skin care after baby is born? (We’ll dive into all these options in more detail below.)
- Even if you know what you want, you may not feel like talking much during labor. Having a plan – and sharing it with your loved ones – keeps you from having to play twenty-questions while in labor.
- Discussing your plan with your OBGYN or midwife before the big day is a good way to make sure you’re on the same page. For example, maybe you want a water birth but it’s against hospital policy, or maybe it’s totally fine and your birth team just needs to know in advance so they can prepare. Either way, it’s important to have that conversation before the big day.
With that in mind, here are 10 questions to consider when creating a birth plan:
1. How do I feel about labor induction?
Inducing labor can be done for elective or medical reasons. More and more hospitals are restricting elective inductions before 39 weeks due to health outcomes, but it’s still an option in most areas. (1)
Although there are definitely times when induction is necessary for medical reasons, more and more care providers are highlighting the benefits of allowing labor to start spontaneously when possible.
Here’s an overview of the benefits of both spontaneous labor (allowing labor to start on its own) and medical induction:
Benefits of waiting for labor to start naturally
According to this study:
In the last weeks of pregnancy, maternal antibodies are passed to the baby—antibodies that will help fight infections in the first days and weeks of life. The baby gains weight and strength, stores iron, and develops more coordinated sucking and swallowing abilities. His lungs mature, and he stores brown fat that will help him maintain body temperature in the first days and weeks following birth. The maturing baby and the aging placenta trigger a prostaglandin increase that softens the cervix in readiness for effacement and dilatation. A rise in estrogen and a decrease in progesterone increase the uterine sensitivity to oxytocin. The baby moves down into the pelvis. Contractions in the last weeks may start the effacement and dilation of the cervix. A burst of energy helps pregnant women make final preparations, and insomnia prepares them for the start of round-the-clock parenting.
The watchful waiting and the intense wanting of the big day to arrive are all part of nature’s plan. When the baby, uterus, placenta, and hormones are ready, labor will start. Additionally, all that preparation sets the stage for an easier labor and a fully mature baby who is physiologically stable and able to breastfeed well right from the start.”
Are there any benefits to inducing labor?
Sometimes, yes. When certain medical conditions such as preeclampsia or heart disease are present, a doctor may determine that it is safer for baby to be born than to remain inside the mama’s womb.
Induction is something that is also often discussed if a woman goes past her due date. However, it’s important to note that:
- Even when the exact day of conception has been identified by researchers – the length of a normal pregnancy can vary by up to five weeks. (2)
- The 40 week due date we all assume is “average” may actually be a little too short. This study and this study suggest that due dates should be calculated to include 40 weeks plus 3-5 days.
- The World Health Organization does not recommend induction in uncomplicated pregnancies under 41 weeks (3)
Is it possible to encourage labor naturally?
According to one study, eating dates during the last few weeks of pregnancy can reduce the likelihood of needing and induction and shorten labor. Here are some more tips for inducing labor naturally.
Are Pitocin and oxytocin the same?
Chemically speaking, oxytocin and its synthetic version, Pitocin, are identical. However, although Pitocin can stimulate contractions like oxytocin and is often used to try to artificially start labor, there are five important differences that affect labor and the postpartum period. Here’s how to increase oxytocin naturally for a better birth and postpartum experience. (These suggestions can be helpful even if Pitocin is needed during or after labor.)

2. Do I want to eat and drink during labor?
No one expects athletes to run a marathon without water, but some hospitals require low-risk laboring moms to do without during the marathon of marathons. When this policy was created in the 1940s, anesthesia procedures were somewhat crude and doctors wanted to reduce the risk of aspiration.
Today anesthesia procedures are much more precise, and a recent review of available studies found no difference in outcomes between women who were allowed to drink during labor and those who weren’t. Actually, there was one small difference – the women who were allowed to eat and drink birthed their babies a little faster than those who weren’t. (4)
According to the American Society of Anesthesiologists:
Without adequate nutrition, women’s bodies will begin to use fat as an energy source, increasing acidity of the blood in the mother and infant, potentially reducing uterine contractions and leading to longer labor and lower health scores in newborns. Additionally, the studies suggest that fasting can cause emotional stress, potentially moving blood away from the uterus and placenta, lengthening labor and contributing to distress of the fetus. ” (5)
There are times when eating and drinking may need to be avoided, such as when eclampsia or pre-eclampsia are present, or if opioids – which delay stomach emptying – are used to manage labor pain. However, for low risk mamas, all these organizations recommend eating and drinking during labor if desired:
- The World Health Organization (WHO)
- The American College of Nurse-Midwives (ACNM)
- NICE Clinical Guidance for the United Kingdom
- The Society of Obstetricians and Gynecologists of Canada (SOGC) (6)
If you decide that you want to eat and drink during labor, here are some snack/refreshment ideas:
Fruit
Nuts and seeds
Energy bars
Popsicles (We love coconut pineapple popsicles and strawberry yogurt popsicles)
Yogurt
Cheese
Veggies and hummus
Labor aid
Coconut water
Red raspberry leaf tea
3. What is the policy on moving freely while in labor?
According to this study, walking, squatting, and even dancing during labor may result in:
- shorter labors
- more efficient contractions
- greater comfort
- less need for pain medicine in labor
That’s because movement often helps open up the pelvis while encouraging baby to move into the birth canal. “Moving or walking can be the perfect tool for pain management — it’s the way your body helps you get through labour,” says midwife Lorna McRae. (7)
That said, not every mama wants to move a lot through labor. For most of my three labors I preferred to lay on my side with a pillow supporting my pelvis, but toward the end I always instinctively got up and started moving around. Every mama is different, and there is no “right” way to labor. However, you’ll want to know whether you’ll have the option to move freely if you want to.
4. What about pain management?
There are a variety of techniques and procedures that can help ease tension throughout labor. Here are a few you may want to discuss with your doctor or midwife:
- Acupressure
- Birth ball – Can help open up the pelvis and help mama find a comfortable position while laboring
- Breathing techniques such as the Bradley Method
- Cool or warm washcloths – Some mamas get very hot while laboring, and a cool washcloth on the forehead can be relaxing. On the other hand, warm washcloths can be placed on the back to ease discomfort during contractions.
- Doula care
- Epidural
- Hypnobabies
- Massage (including techniques like counter pressure and hip squeezes)
- Meditation
- TENS unit
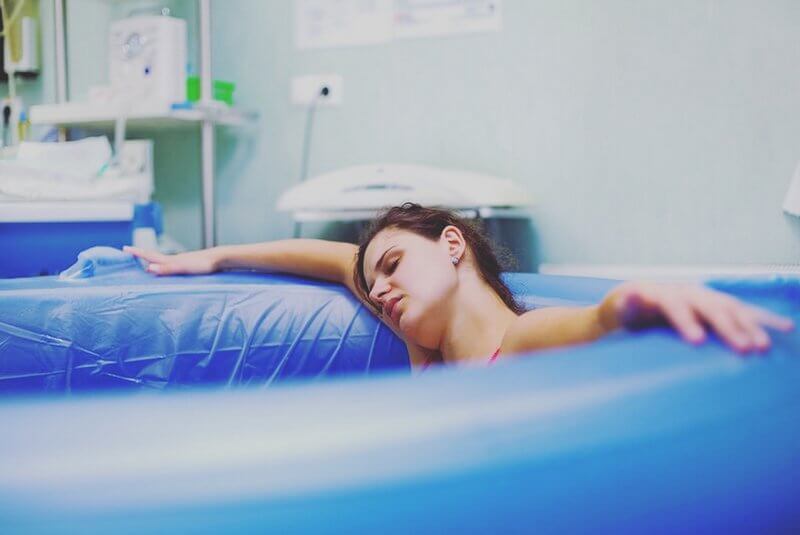
- Warm water to labor in
5. How do I plan to give birth?
- Vaginal birth
- Gentle caesarean
- Water birth
- VBAC
6. Do I want continuous fetal monitoring or intermittent?
Continuous electrical fetal monitoring (EFM) is standard practice in many hospitals, but research says that “based on the evidence, intermittent auscultation [monitoring] is safer to use in healthy women with uncomplicated pregnancies than electronic fetal monitoring (EFM).” (8)
With continuous monitoring, the risk of newborn seizure drops from 0.3% (very rare) to an even more rare 0.15%. However, according to Rebecca Dekker, RN, PhD, the risk of cesarean section, vacuum/forceps delivery and an increase in perceived pain all go up. She covers the research on both approaches here. Scroll to the very bottom of the post for a helpful list of pros and cons.
Other considerations: Moms used to have to choose between freedom of movement and continuous electrical fetal monitoring (CFM), which required moms to be hooked up to a machine and stay in bed. Things have changed recently with the introduction of wireless fetal monitors, however not all moms are comfortable with continuous monitoring due to the increase in EMF exposure.
Other options, such as a fetoscope (stethoscope designed to listen to a baby’s heartbeat) can also be used for hands-on listening (monitoring at regular intervals).
7. Who will be in the room with me?
Do you want certain family members, a doula, and/or a birth photographer? What about the baby’s siblings?
A couple of notes: I wasn’t sure how my children would react when they saw me in labor, so I asked a trusted friend to care for them and take them out of the room if they seemed uncomfortable. My oldest loved being present for both of her siblings births, but my middle child was not all that interested in the birth of my youngest.
Also, if you’re birthing at a hospital or birthing center, make sure photography and/or videography is allowed during labor.
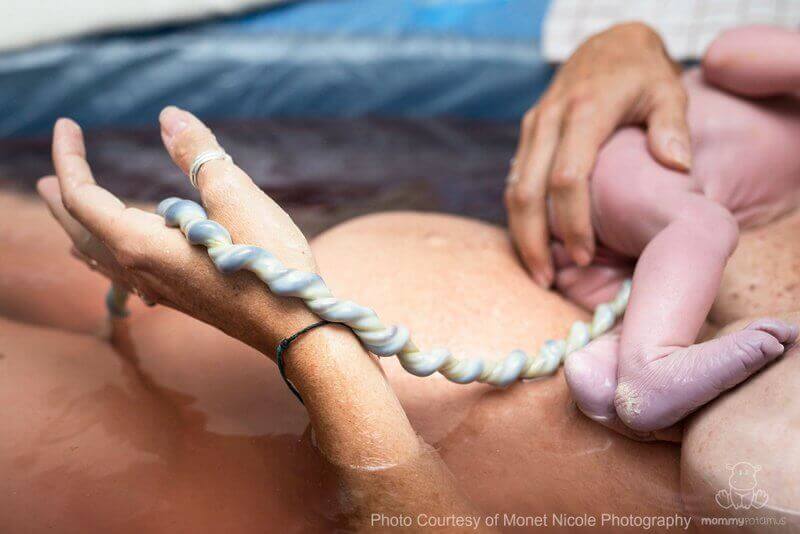
8. What about delayed cord clamping?
Delayed cord clamping is becoming the standard of care in many hospitals, and for good reason.
“It’s incredible to see what a difference an extra three minutes and one-half cup of blood can have on the overall health of a child, especially four years later,” Dr. Ola Andersson told CNN. She was the lead author of a study that found delayed cord clamping resulted in neurodevelopmental benefits for preschoolers.
Delayed cord clamping or cord milking is sometimes possible when baby is born via cesarean section. Read more on the benefits of delayed cord clamping here.
Note: Although delayed cord clamping is usually not considered compatible with cord blood banking, some sources say it is compatible if the cord is allowed to pulse for 1-3 minutes. (9)
Another option to store a child’s stem cells for later therapeutic use is to bank a baby tooth when it comes out. Unlike cord blood which has a limited number of therapeutic uses, the stem cells found in tooth pulp have a wide variety of potential uses. I’ll be writing more about that soon.
9. Do I want to be skin-to-skin with my baby right after birth?
Babies benefit immensely from skin-to-skin care in the moments after birth. When it’s not possible, or even when it is, mamas should know that it’s also beneficial in the days, weeks, and even months after baby arrives. Here’s your guide to getting started.
10. Do I want to keep my placenta?
Some women opt to encapsulate their placentas for postpartum support. For many, placenta encapsulation benefits mood and energy levels by delivering oxytocin, thyroid stimulating hormone, interferon, prolactin and several other components.
Considerations for c-sections (planned and unplanned)
For some mamas, a c-section birth is a thoroughly considered, planned event. Even if it’s not, “a good plan shouldn’t just describe your best-case scenario; it should also include your preferences in the event that things don’t go according to plan,” writes Genevieve Howland in The Mama Natural Week-by-Week Guide To Pregnancy & Childbirth.
“I’d known long before I got pregnant that I wanted a vaginal birth, but I also knew there was always a chance of having a C-section,” she continues. “That’s why my first birth plan included my preferences in the event that I ended up in the OR. (My highest priorities? Immediate skin-to-skin contact and immediate breastfeeding, if at all possible.) Nobody wants to think about all the things that could go wrong during delivery, of course, but you also don’t want to be making important decisions in between contractions (for obvious reasons!).”
I highly recommend Genevieve’s book, and two other helpful resources on this subject are:
Creating Your Written Birth Plan
If you’ve answered the questions above and are wondering how to put it all together into a written plan, check out this post from my friend Genevieve. She’ll show you how to create a one page birth plan that practitioners won’t scoff at.

Want to learn how to have an awesome birth without leaving your couch?
If you’re looking for an evidence-based, naturally-minded resource, I highly recommend the Mama Natural Birth Course and/or The Mama Natural Week-by-Week Guide to Pregnancy and Childbirth.
You’ll learn about:
- Delayed cord clamping, which boosts baby’s iron stores by 30% and improves fine motor skills and social development later in life.
- Skin-to-skin contact, which regulates baby’s body temperature and blood pressure, reduces stress hormones, and helps initiate early breastfeeding.
- Gentle cesarean, which can “seed” baby’s microbiome, eliminate fluids from baby’s lungs, while empowering the mama.
- The importance of eating during labor, and so much more.
Click here to check out the Mama Natural Birth Course, and here to check out The Mama Natural Week-by-Week Guide to Pregnancy and Childbirth.
Article Sources:
1. Associated Press/NBC News (2009) Hospitals to crack down on induced labors. Retrieved from NBCNews.com
2. Cooper, Charlie (2013) Length of pregnancy can vary by up to five weeks, scientists discover. Retrieved from Independent.co.uk
3. World Health Organization (2011) General principles related to the practice of induction of labour. Retrieved from PubMed
4. Ciardulli, A et. al. (2017) Less-Restrictive Food Intake During Labor in Low-Risk Singleton Pregnancies: A Systematic Review and Meta-analysis. Retrieved from PubMed
5. American Society of Anesthesiologists (2015) Most healthy women would benefit from light meal during labor. Retrieved from ASAHQ.org
6. Dekker, Rebecca (2017) Evidence on: Eating and Drinking During Labor. Retrieved from EvidenceBasedBirth.com
7. Pitman, Teresa (2009) The secret to an easier labour. Retrieved from TodaysParent.com
8. Heelan, Lisa (2013) Fetal Monitoring: Creating a Culture of Safety With Informed Choice. Retrieved from PubMed
9. Americord. Delayed Cord Clamping: A Guide to Research and Options. Retrieved from AmeriCordBlood.com









