
Hey mamas! After Micah was born I found myself reading his story over and over, but Katie’s sat untouched in a dusty corner. It’s was a “just the facts, ma’am” catalog of timestamps and pushing techniques . . . pretty much a total yawner. Now, I LOVED her birth, it was just that my story didn’t do it justice. So here is my second attempt: Elvis and Smurfs included for dramatic effect 🙂

In my bedside table there is a calendar with your conception date circled on it. That is a fact. Doing the potty dance in the Walgreens checkout line while holding a pregnancy test was just a formality . . . I knew you were there three days in when I ate an entire jar of olives and drank the juice!
And because I did the math – oh, about a thousand times – I can tell you it is also a fact that your due date was December 8th.
So when December rolled around I washed your little onesies and yellow ducky receiving blankets (we didn’t know if you were a boy or girl), made snacks for my birth attendants (which I, um, ate before they arrived), and waited.
tick. tick. tick.
tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick.
Now Honey . . .
As much fun as it was to watch the gym staff clutch their chests as I heaved my planet-sized belly onto the stairmaster at 41 weeks, I was beginning to think we had a problem. A huge, 25th of December type problem. As you know, mama LOVES Christmas, but I couldn’t shake the feeling that I’d stuck you with a lemon of a birthday. Not ON Christmas, of course, but just close enough that your big day would be swallowed up in the hullabaloo. Now that I’ve gotten to know you a bit I see how silly this was. I mean, who could ignore this?!?!?

But I am getting ahead of myself. On the morning of Dec. 21, which was the final day of week number 42, you started revving things up around 6am. Of course, I promptly did what any reasonable laboring mother would do . . . I put rollers in my hair and grabbed my eyelash curler! A few days before I’d done a glam birth trial run, so I was pretty sure I had this in the bag.

Please feel free to skip ahead a couple paragraphs and laugh yourself silly at my naivete! So where were were we? Oh right, go time! I spent the morning wrapping Christmas presents and trying to stay relaxed. Then around midmorning my STRONG hypnobirthing “pressure waves” subsided into tiny ripples that barely lapped the shore. I was devastated, but now I’m glad I got a little rest before stage two.
Stage 2: Puke-A-Thon
So here is the thing about glamorous births: They do NOT involve heaving everything you’ve eaten since 1987 into a giant mixing bowl.
For 12. hours. straight. Current theories on how I was able to find enough stuff in my stomach to vomit after every other contraction include:
- I can metabolize air
- It was not really 12 hours, but one hour which I experienced Groundhog Day style (this conspiracy theory is patently false)
- I am Elvis
Whatever the true cause, my glam birthing clothes are covered in slime and I now have this ratty old t-shirt on.
By this point I’ve been awake for over 24 hours and haven’t been able to keep food or water down for half of that. I’m beyond weak and terrified that I don’t have the strength to finish. My midwives, Susan (aka The Urban Poser’s MIL) and Angela are becoming concerned for the very same reason.
Game Face? Check!
I needed some space from all the eyeballs gazing at me with deeply concerned expressions, so I took a shower. My family took this opportunity to hold full-on Sunday-go-to-meetin’ prayer extravaganza. They knew something had to happen or I was going to end up at the hospital with an emergency c-section.
Standing in the shower, I knew it too. But as steam swirled all around something changed. I was ready and willing to trust my body. My expectations of a picture-perfect birth with neatly coiffed hair and just the right shade of lip gloss were replaced by sweat and puke. But I was ready. Instead of running from the pain I started leaning into it, using this excruciatingly painful maneuver to cause myself to dilate. It worked.
Now, a funny thing about midwives is that they speak grunt. “Mhmmpf” means someone please hand me one of those oatmeal creme pies. But “Mmmmmmhmpf” is best translated as “fill the birthing tub now or I will have this baby standing up.” Since I’m clearly saying the latter by this point they fill the tub and help me in.
Ahhhhhhhhhhhhhh! After 35+ hours of labor this was exactly what I needed. Unfortunately I must have let out a “Ohmmpf,” which unbeknownst to me means “get me out of the tub so I can push on the toilet,” so out I came.
Oops.
Sitting backwards with my forehead on the tank did help, though, so I guess the midwives grunt translator is pretty accurate. Or maybe the Smurfs told them. Hey, who invited Smurfs to my birth!?!?!?
Susan didn’t see the Smurfs, but that’s probably because her perception had been dampened by the fact that she’d slept in the past 40 hours. Or I hallucinated them. Whatev.
So Here We Are . . .
Past the glam curler phase, the puke vortex and the Smurf interlude. I guess the only thing left is to push you out! Susan and Angela led me back to the birthing tub where your dad was waiting. I pushed, and pushed, and PUSHED, but all I got was a bulging bag of waters. Finally in desperation I asked my midwife to break it. The first tried and couldn’t, but the second was finally able to. (Susan later told me that my amniotic sac was incredibly strong because of the way I’d nourished myself through pregnancy. Yay me!)
With one gush I passed into the eye of the storm. Everything around me was suspended, and my only thoughts were of you. I felt no pain as you passed through, and as your Daddy gathered you up from the water I leaned back, exhausted. They laid you on my chest and I gazed at you in stupified amazement.
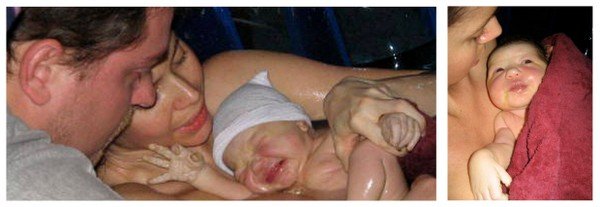
All through my pregnancy I had eaten well, exercised, etc. I had done everything I could to take care of you. But the moment I saw you I was totally undone. Your pink cheeks, rosebud mouth and tiny frame melted me into a puddle of awe. Finally your dad said “Well, what is it?” I had forgotten to check! We pulled back the towel and I yelled “It’s a GIRL!!!” just like in the movies.

We snuggled into a freshly-made bed and nursed while the midwives examined my placenta. Someone put a diaper on me and that was that. We were officially a family of three.
You were born three days before Christmas, and for years I felt guilty about it. But you know what? Your birthday is only time the sun rises and sets in the same place. Oh yes, little one, you are a Winter Solstice baby – wrapped in the paradox of a sun that appears to stand still right before the longest night of the year. From that day forward the days grow warmer and brighter until midsummer when all settles down for a quiet rest again.
The longest, darkest night followed by light and warmth? Yes, that sounds vaguely familiar! And that, sweet girl, is why I will never feel guilty about your birthday again. Indeed, it is the only day fitting for you.





As an older Winter Solstice baby I have to say we have the *best* birthday ever. And we tend to have funny birth stories and incredible mamas to punctuate that fact.
Thank you. 🙂
Wonderful! Loved it!!! 🙂
Absolutely wonderful birth story! Loved it and the humor was great. 🙂 What an awesome mama and baby! 🙂
Glad you liked it, John and Emily!
I love this birth story. If it’s ok, I think I am going to print it to give to all my future doula clients. It is very in-tuned of you to realize that it is necessary to “let go” in order for birth to proceed. “Instead of running from the pain I started leaning into it, using this excruciatingly painful maneuver to cause myself to dilate. It worked.” It is that very idea that I try to convey to my laboring mommas… and your story demonstrates it and elaborates on it very well 🙂 So thanks!
I would be honored for you to share my story, Hannah Landis. Thank you <3
I love it. What a great way to tell the story. (:
I love this – it reminds me so much of the birth of my first daughter, especially the puke a thon lol. However, I had mild, but regular contractions for 2 weeks before while serious “I’m in labor” labor lasted only 4 hours start to finish. I think it’s cause I took Dr. Christopher’s prenatal formula during the six weeks before. Everybody I know who tries this says it makes a HUGE difference with their labors. Gotta love those herbs!
I did a gentle birth formula with both kids but I think my labors progress differently due to some kind of structural thing (both were asclyntic). Maybe next time I’ll try Dr. Christopher’s to see if I can tell a difference!
I so wish I had heard of that maneuver before my second son was born! We actually were totally sure whether he was a brow presentation, or just had his hand up by his head. My midwife’s first thought was brow, but she wasn’t sure and that is much more rare than a hand. He was born by c/s with a huge puffy ring on one side of his forehead. I didn’t know until about 8 hours into labor that his presentation was off, and I wasn’t really going to settle down and the computer at that point! Now I am wondering if he had dropped/ was engaged in the pelvis, and if my midwife should have known something was up from that. My labor started with my water breaking a week before my due date, though, so who knows.
Wonderful birth story! My son(baby #4) was born this past winter solstice too, “late” by over a week. There is something really special about December 22nd!
I totally agree, Sarah! I never thought I would LOVE that she was born 3 days before Christmas, but I totally do!
Heather,
Hello Hello! I absolutely love love love your blog! And I don’t even have kids, but it is so well written and so informative and thought provoking! I am so happy I found you/it via Pinterest. Thank you for sharing.
Rachel, did you happen to go to high school in Hurst, TX? I think I know you 🙂
Oh and my husband was born on Christmas Eve! ; )
I loved reading this! The mmph part had me laughing.
Oh my lovely ~ what a great story! I too devoured olives and juice….and continued to do so for the first trimester. Do you elaborate any where else in your blog about the structural abnormality? My first babe was asclyntic too; and as we plan for a second I am crossing everything I’ve got that that presentation does not repeat! 🙂 I just submitted our story; I was all over the room trying to get my girl to move down and out.
Thanks again for sharing! Your Solstice girl is breath-taking!
I don’t know if it is an abnormality or the fact that I unintentionally stalled labor with Katie by being unwilling to get moving and then intentionally stalled it with Micah to give him the birthday I wanted. I kind of think it was just that things got out of whack because I didn’t fully work with my body, but we’re hoping for a third so I guess I’ll get to test that theory!
I’m very sure this wasn’t as much fun to go through as it was to read…. I’m still giggling at the thought of putting rollers in your hair when you realized you were in labor. (Or, more precisely, giggling at my husband’s reaction if I’d ever tried to do that. lol)
What a lucky girl to have a story like this to read when she grows up! : )
A friend of mine posted a link to your story on Facebook. What a great story! I am getting ready to celebrate the birth of my Winter Solstice baby–he’ll be 16 tomorrow. The best Christmas present ever!
I love this! I used that excruciating move as well, with babe number two. Holy pain, batman!! Got #3 in the oven right now, due date: winter solstice. 🙂
Awwww, CONGRATULATIONS Faith! So happy for you!
Thank you for sharing this amazing and beautiful story of your birthing experience. I know how you felt about the whole Christmas thing. My daughter ended up coming on 12/29 and they day fits her well! There is no confusion separating her birthday from Christmas in this house 🙂
Awesome Beautiful story! VERY similar story to my own Winter Solstice baby who was stuck so long he ended up coming on the 23rd…ouch! 🙂 I never did make it into my tub for a waterbirth….at least I did with my 2nd – congrats on baby #3!!!
Hi Heather, I’m new here. I loved reading your birth story for your daughter. It so reminded me of the birth of my first, also a little girl. After two days of labor and SIX hours of pushing, my midwives thought I may have to head to the hospital for a vacuum or c-section birth. But, where there’s a will, there’s a way. After two hours of toilet sitting pushing, our daughter was born on the bathroom floor, 8.5 lbs! I thought in was the only one who has ever gone through 30+ hours of labor. And btw, you looked just fine in your old t shirt! – Bernadette 🙂
Ha, thank you! I’m so glad you got the outcome you wanted!
Great birth story, you tell it well. My husband’s birthday is the day after Christmas and he has always felt uncelebrated (who has any energy to celebrate the day after Christmas?). Three days before Christmas, though, is a great birthday! And Susan and Angela were my midwives too, I just love them!
I was working hard too, 4 years ago! Tomorrow is her birthday!
I’m a solstice baby. 🙂 (well grown up baby now lol)
Awesome! Austin is a solstice baby too….3 years today!
My current youngest turns 2 today!
My baby turns 2 tomorrow!
Love it!! I have a dec 18 baby girl:) i love christmas so she was my best christmas gift
My girl is 3 tomorrow!!
I’m a solstice baby, but in Brazil it’s summer solstice 😉 today is a great day to arrive 🙂 congrats to all solstices
That was me last year! My little girl turns one tomorrow. By this point last year I had been in labour for 26 hours already. I went into the labour whilst watching The Hobbit at the cinema and freaked my husband out because I refused to leave until it was over despite my contractions!!!xx
Mine turned 14 today. I would have loved to have a waterbirth but that was not available to me then. Plus she was my first and I had no clue what was to come.
I’m hoping to be working to meet my little miss today, but we will see…
My hubby is a solstice baby 😉
Lol, Charlotte Bulman!
Happy Birthday Katie!
So elequent and humorous, too! 🙂 I love it!
Such a beautiful story. Brought tears to my eyes
My first boy is 10 today. My second boy is 10mths. Both born on my lucky 21. 12-21 and 2-21 🙂
.
Wow, Angie! So neat!
8:56 am tomorrow!!! My little boy is 3!
Mery Flabia Torres
I was working hard too 25 years ago tomorrow. Right after midnight. Greatest joy in my life. My first son.
My baby girl is 9 years old today! And last year today we found out we were having twin girls! 🙂
Thanks for sharing your beautiful birth story! I very much enjoyed it .
13 yrs ago yesterday I was working hard too, to change my life from a carefree- just turned 21 yr old to a MOM. I wish I had the know all that I do now, but my journey with my son is where it all started. I sit and look at his mini me that is 3 mnths old and it almost feels like déjà vu. Happy birthday Christmas babies! ( oh and I learned never to have a December baby again! Poor kid lol)
So well shared! Thank you! As a blessed Mama of 4 drug free (amazing!!) births (2 home, 2 birth center) I could picture each event and smile 🙂
My first is 3 today. Born during a lunar eclipse! Love my girl.
(At home)
This is beautiful!
Especially enjoyed the ending.
Awww! My first born will be 4 tomorrow. Sounds very similar to my story. Happy celebrations and day of birth to our loves and us :0)
Very funny Mommypotamus. Thanks for sharing.
What a sweet story 🙂
So sweet <3 <3 Thanks for sharing.
Yeah, I went into labor with my first the day BEFORE my due date and had her the day AFTER. I understand the long labors! Happy Birthday to you as a Mama and your sweet Daughter! We celebrate 5 years in February. 🙂
I remember the day well- love y’all!
Wow!! I’m so glad you had such a positive experience.Thanks for sharing
My daughter too was born on the solstice….I hated the late December birth for her, until I realized how very fitting it was! I am a Dec. 12th baby and was so upset she was born on the 22, but you are right it is fitting!
Dec 8 was my due date, too! I was worried about a Christmas baby, but he surprised me and came on the 2nd.
And, I somehow need to rewrite his birth story as well. It’s very factual but leaves out all of the emotion. Thanks for the inspiration!
I love how you brought out the birthing story after setting it aside for a time. You found all the dark moments and turned them into a beautiful memory. Thank you for reminding us to step back and find the beauty. (This is so well written – just reading this story makes me want to have another baby!)