Two pink lines. I remember where I was standing the first time I saw them, and how I immediately started looking forward to my first ultrasound. I wanted to know everything was okay and connect with this little being that was going to grow to the size of a watermelon and . . . well, let’s just say that as my train of thought continued along those lines I completely forgot about the ultrasound for awhile.
When I did finally mention it to a friend, she gently suggested that I might want to research a little more before getting one without a clear medical need to. I did, and what I learned surprised me. Here’s why:
- Routine prenatal ultrasounds have not been shown to improve outcomes for mothers or babies. (1) (2) (3) (4)
- No major epidemiological studies have been conducted on the safety of prenatal ultrasound within the U.S. in over 25 years.
Before we go any further, know this: I am not against the use of prenatal ultrasounds and think there are times when they are incredibly valuable. With that said, every mama should be fully informed about the potential risks and benefits of having one, or two, or six based on her unique situation. That’s why in this post we’ll cover:
- What peer-reviewed research says about the safety of ultrasound
- The effect of routine ultrasounds on birth outcomes
- What conditions ultrasounds can screen for (and alternative test options when available)
- Steps to limit exposure when ultrasounds are needed or wanted
After reviewing the research I chose to be selective about the use of ultrasound during my pregnancies, opting for one only if medically indicated. Your approach may be different, and I completely support that.
Also, please keep in mind that “Boo Boo Kisser” is about as official as things get for me professionally. I am not a doctor and this is not medical advice. Now let’s dive in.
- What is a prenatal ultrasound?
- What’s the difference between a sonogram and ultrasound?
- What are prenatal ultrasounds used for?
- Do routine ultrasounds improve birth outcomes?
- Lessons Learned From Prenatal X-Rays
- The Problem With Most Ultrasound Safety Studies
- So what are the potential risks of prenatal ultrasounds?
- Is it possible to minimize the risks of sonograms?
- The decision to have an ultrasound (or not)
- Did you have a prenatal ultrasound?
- Want to learn how to have an awesome birth without leaving your couch?
What is a prenatal ultrasound? ^
Originally developed by the military to detect submarines via SONAR, ultrasound technology bounces ultra high frequency sound waves off the soft tissues and bones of a baby in the womb, then uses the pattern created by the different surfaces to generate an image.
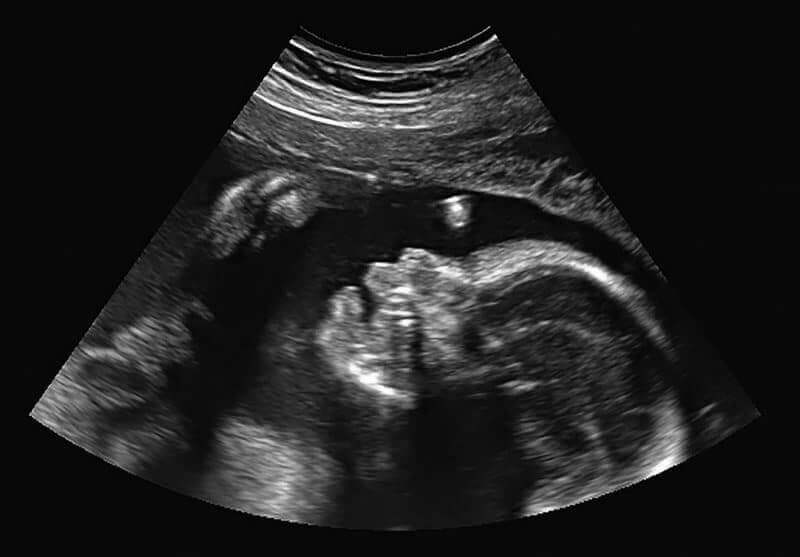
What’s the difference between a sonogram and ultrasound? ^
Ultrasound is the technology used to create the image, and a sonogram is the picture created using the information gathered by the ultrasound. Not all ultrasound technologies generate an image, though. The fetal doppler, for example, is used to listen to baby’s heartbeat without generating a picture. Here’s an overview of the seven types that are most often offered during pregnancy:
- Standard Ultrasound – Creates a 2-D image by moving a transducer (wand) over the abdomen area.
- Advanced Ultrasound – This is similar to the standard ultrasound, but the exam targets a specific area or organ system using more advanced equipment.
- Transvaginal Ultrasound – Creates a 2-D image via a probe that is placed inside the vagina.
- Fetal Doppler (audio)- Some say this form delivers a lower level of exposure than other forms, but others say it is more likely to heat tissue (one of the concerns with ultrasound) when used for more than a brief period because handheld fetal dopplers typically use continuous waves instead of pulsed waves.
- Wireless or Mobile Electronic Fetal Monitoring– Primarily used to monitor a baby’s heart rate during labor. Other options, such as a fetoscope (stethoscope designed to listen to a baby’s heartbeat) are also available.
- 3-D and 4-D Ultrasound – The FDA has warned consumer to avoid these two types of “keepsake” ultrasound because the individual performing them may use higher power settings and longer exposure times to get a “good” picture.
What are prenatal ultrasounds used for? ^
Although there can be specific reasons related to an individual concern, ultrasounds during pregnancy are most often used for:
1. Dating the pregnancy
If a mama knows when her last period was or the date of conception, her due date will usually be determined from that. However, if she is not sure when her last period was or has very irregular periods, her care provider may recommend an ultrasound to determine how far along she is.
An ultrasound to determine gestational age is most accurate when done early in the pregnancy – between 8 and 11 weeks. (5)
However, not everyone agrees on the benefit of dating ultrasounds. A review of the literature published in Midwifery Today concluded that using early dating ultrasound to determine when a pregnancy exceeds 41 weeks does not improve birth outcomes. (6)
This may be because:
Although it has always been known that human pregnancies usually last between 37 and 42 weeks, the variation has previously been attributed to imperfect methods of estimating due dates.
. . . However researchers from the National Institute of Environmental Health Sciences (NIEHS) were able to pinpoint the moment women became pregnant by taking daily urine samples – enabling them to isolate the role that natural variation plays in pregnancy length.” (7)
They discovered that even when they knew the exact date of conception, the length of pregnancies varied by up to five weeks.
‘We were a bit surprised by this finding, said Dr Anne Marie Jukic, a postdoctoral at the Epidemiology Branch at the NIEHS. ‘We know that length of gestation varies among women, but some part of that variation has always been attributed to errors in the assignment of gestational age. Our measure of length of gestation does not include these sources of error, and yet there is still five weeks of variability. It’s fascinating. ” (7)
2. Screening for nuchal translucency and heart defects
During the first trimester, another ultrasound is often offered in combination with two blood tests to screen for chromosomal abnormalities (specifically Down Syndrome and Edwards Syndrome) and heart defects. The results are not usually considered diagnostic, but they may indicate if there might be an issue that needs more careful evaluation via additional (more invasive) tests.
How accurate is this screening? According to one French study, 8.8% percent of the problems identified by ultrasound were incorrect (false positive). “The false-positive rate during prenatal ultrasound is not insignificant,” they concluded, noting that it causes significant stress for the parents and can lead to additional medical interventions that have the potential to cause harm due to their invasive nature. (18)
There’s also the potential for false negatives, which indicate a normal result when the baby actually does have a chromosomal abnormality. For example, “20% of women with pregnancies affected with Down’s syndrome will receive a screen-negative result.” (8)
Is there an alternative screening tool? For several of the conditions screened for, the answer is yes. In 2011, a non-invasive blood test called cell-free fetal DNA testing became available which determines the likelihood of a baby having Down syndrome, Edwards syndrome (trisomy 18) or Patau syndrome (trisomy 13).
It’s considered highly accurate for Down syndrome – with a false positive and a false negative rate of less than 1% – but when the other syndromes are considered it’s accuracy is between 91-99%.
Again, like an ultrasound, it is considered a screening tool and not a diagnostic tool. The only diagnostic tests available are amniocentesis and chorionic villus sampling, which are more invasive procedures that carry more risks. While the cell-free DNA testing is less invasive, it should be noted that it does not screen for heart defects.
MaterniT21 was the first to offer this test, but other companies have also made it available.
3. Anatomy ultrasound
Even if you’ve never had an ultrasound, I’ll bet you’ve seen so many in movies that you can almost hear the squirt of the gel as it is placed on a pregnant woman’s belly just before the machine is turned on. Of all the ways we depict pregnancy in our culture, the 20-week anatomy scan is one of the most well-known.
It makes sense, of course: The 20-week anatomy ultrasound is joyful for a lot of parents because it’s usually when they find out the sex of their baby, although now the cell-free fetal DNA test mentioned above can determine sex at around 10 weeks. (You can also opt not to find out if you prefer.)
From a screening perspective, this ultrasound – which is usually around 30 minutes – is used to look for genetic abnormalities and congenital defects, check amniotic fluid levels, and check the position of the placenta.
4. Checking for a “big baby”
Sometimes an additional ultrasound is recommended in the third trimester to check for macrosomia, or a suspected “big baby.” However, determining fetal weight is notoriously inaccurate – the estimated error rate in both directions is 15%, meaning that the baby may be 15% smaller or larger than predicted. However, some moms report that their baby’s predicted weight and actual weight were more than 15% apart.
How likely is a big baby? In The Mama Natural Week-by-Week Guide To Pregnancy & Childbirth, Genevieve Howland explains:
Less than 2 percent of newborns in the US exceed 9 pounds, 5 ounces. Despite your slim chance of delivering a hefty baby, however, you’ve got a relatively high chance of being told that your baby is “too big.” A 2013 survey of new mamas revealed that 1 in 3—or 32 percent —were warned about this very possibility, but the average weight of their supposedly enormous babies at birth turned out to be . . . wait for it . . . less than 8 pounds.”

Do routine ultrasounds improve birth outcomes? ^
Many healthcare providers consider the anatomy ultrasound (and sometimes other ultrasounds) part of their standard of care even when no problems are suspected. Do these “routine” ultrasounds actually improve outcomes for mama and baby? Somewhat surprisingly, the answer is no.
According to this meta-analysis, “Routine scans do not seem to be associated with reductions in adverse outcomes for babies or in health service use by mothers and babies.” Several other studies support these findings.
A review of the literature also concluded that using ultrasound for second trimester organ scan, biophysical profile, amniotic fluid assessment, and Doppler velocity has been “somewhat able to detect findings of questionable relevance but unable to improve outcomes.” (6)
Ultrasounds are fairly accurate for detecting placenta previa, but over 90% of cases that are diagnosed in the second trimester will resolve on their own by 34-35 weeks. (9) It’s a relatively rare condition – only 0.4% of mothers in this large study had it in the third trimester – and in most cases women have symptoms that can lead to diagnosis.
Not all women have symptoms, though, and there are factors that increase the likelihood of having placenta previa that doesn’t resolve – having a previous cesarean and being pregnant with multiples are two examples. Fortunately, as the imaging clarity of ultrasound technology has increased, it’s become possible to better identify which cases of placenta previa are more likely to persist.
Unfortunately, the flipside of that is that the intensity of the ultrasound is also higher – much higher than what was used in safety studies. That’s important to note because according to the Guidelines and Recommendations for Safe Use of Doppler Ultrasound in Perinatal Applications:
When modern sophisticated equipment is used at maximum operating settings for Doppler examinations, the acoustic outputs are sufficient to produce obvious biological effects, e.g. significant temperature increase in tissue or visible motion of particles due to radiation pressure streaming effects. The risk of inducing thermal effects is greater in the second and third trimesters, when fetal bone is intercepted by the ultrasound beam and significant temperature increase can occur in the fetal brain.
Transvaginal probes are typically used instead of doppler technology for checking placenta previa, but the same principle applies.
Lessons Learned From Prenatal X-Rays ^
When Oxford physician Alice Stewart began investigating the alarming rise of childhood cancer in the 1950s, she had a bold idea: She would ask the mothers. Dr. Stewart believed mothers are tuned into details that doctors might overlook.
Only 35 questionnaires in, the pattern was clear.
Too many boiled sweets? No. General risks associated with low-income? No – in fact the children that were affected came mostly from wealthy families. Only one thing stood out, and it was that most of the children who developed leukemia had undergone a single diagnostic prenatal X-ray, well within the exposure considered safe. With this brief exposure, their risk of cancer nearly doubled. (10)
As parents, I think we’d all hope a finding like this would lead to follow-up research and a change in treatment practices if needed. Unfortunately:
Radiography was medicine’s new toy and was being used for everything from examining the position of the fetus to treating acne and menstrual disorders. It was even used in shoe shops: children loved to watch through the x ray machines while they wriggled their toes in their new shoes. (11)
So instead of digging deeper, the International Commission for Radiation Protection (ICRP) and other organizations disputed her findings.
The data was out there, it was open, it was freely available, but nobody wanted to know. . . . Alice Stewart had a very big fight on her hands,” said Margaret Heffernan in a recent TED Talk.
Funding for her research was cut off, but she continued to fight. She was publicly ridiculed by her colleagues, but twenty-five years later the medical community finally acknowledged her research and abandoned the practice of using x-rays on pregnant women. (12)
What’s the takeaway here? For me, it’s that sometimes it can take decades for concerns to be validated or invalidated, and in the meantime it is up to us as parents to make the most informed decision we can.
I believe ultrasound can be an incredibly valuable tool – and have personally opted for a prenatal ultrasound when medically indicated – but I’ve also consistently requested that my care provider use the lowest setting and the shortest scan time possible to get the information we were seeking.
This is called the ALARA (As Low As Reasonably Achievable) principle – we’ll talk more about it later in this post.
The Problem With Most Ultrasound Safety Studies ^
If you head over to PubMed and start looking around, you’ll find that no major epidemiological studies have been conducted on the safety of prenatal ultrasound since the early 1990s. Well, not in the West at least . . . there are human in utero exposure studies coming out of China which suggest possible adverse effects, but most have not been translated yet, and the few that have usually just contain the title and a brief summary without the study details.
So let’s take a look at the research we do have access to. There are two significant problems with the older “gold-standard” randomized, controlled human studies that are still cited today:
1. Different Intensities
Ultrasounds are often assumed to be safe because some early human epidemiological studies reported no difference between scanned and unscanned groups other than a higher incidence of left-handedness in boys. Left-handedness is normal for some children, but according to Sarah Buckley, M.D. a higher-than-normal incidence can be a “marker of damage or disruption to the developing brain.” (13)
The equipment used in these studies was made before the mid-1990s, their acoustic output upper limit was 94 mW/cm2. Ultrasound devices now in use can have an acoustic output of up to 720 mW/cm2, which is eight times higher.
“If you put more power into the body, more can be absorbed,” says Phillip Bendick, PhD, RVT, FDMS, technical director of the Peripheral Vascular Diagnostic Center and director of surgical research at William Beaumont Hospital.
He also notes that a main heat-absorbing structure in a baby is the spine, which is near delicate neurologic and vascular structures. (14)
2. More Scans And Longer Scan Times
As the intensity of ultrasound machines has increased, so have the number of ultrasounds received.
In the mid-1990s – which is around the same time the original studies were conducted – the average number of ultrasounds a pregnant woman received was 1.5. (15) That number climbed to 5.2 in 2014 and continues to increase. (16)
Also, some of the studies which showed no effect used very short exposure times. This one, for example, used a 3 minute exposure versus the typical 30 minute one most women receive.
So what are the potential risks of prenatal ultrasounds? ^
There are so many studies available, many which suggest caution. Here are some of the most significant:
Yale Researchers: Ultrasound Causes Brain Abnormalities In Mice
In this study headed by Dr. Pasko Rakic of Yale University, researchers found that mice who were exposed to 30 minutes of continuous ultrasound in utero showed altered neural development. Usually, neurons created in the cortex travel to the outer part of the brain, where they help with language and memory. When exposed to ultrasound, some of the neurons remained scattered throughout the brain instead of making it to their final destination.
Dr. Rakic noted that “the ultrasound parameters and total exposure time are comparable with or below those used by commercial medically nonindicated prenatal ultrasound videos.”
Now, it’s tempting to think “But those are mice. Mice aren’t people!” However, there’s a good reason to pay attention to this study.
According to this article in Midwifery Today, neurodevelopmental defects in rats and other mammals should be of concern to expecting mothers “Because, as Cornell University researchers proved in 2001, brain development proceeds in the same manner ‘across many mammalian species, including human infants.’ The team found ’95 neural developmental milestones’ that helped them pinpoint the sequence of brain growth events in different species.(15) Therefore, if repeated experiments show that elevated heat caused by ultrasound damages fetal brains in rats and other mammals, one can logically assume that it can harm human brains, too. (3)”
Decreased Sociability And Hyperactivity
This study concluded “that exposure of juvenile mice in utero to thirty minutes of diagnostic ultrasound can cause them to exhibit autistic-like behavior, specifically social deficits and hyperactivity in social circumstances.”
Here are a few additional studies that Dr. Buckley mentions in Gentle Birth, Gentle Mothering:
- “A large UK study found that healthy mothers and babies randomized to two or more Doppler scans to check the placenta, beginning in midpregnancy, had more than double the risk of perinatal death compared to babies unexposed to Doppler. (66)” (13) (emphasis mine)
- Another Australian study suggests that Doppler ultrasound may actually increase the likelihood of developing a condition it’s used to detect. Babies who were randomly selected to receive “five or more Doppler ultrasounds during pregnancy were more likely than babies . . . [randomly selected to receive] . . . routine (pulsed) ultrasound to develop intrauterine growth retardation (IUGR) – a condition that ultrasound is often used to detect. (64) This may be related to higher exposure levels with Doppler, as more IUGR has been found in high-exposure animal studies, but not in lower-exposure human studies using pulsed ultrasound.” (13) (emphasis mine)
- Also discussed are several “Single or small studies that have shown that possible adverse effects include . . . preterm labor or miscarriage (26) (62), low birth weight (63) (64), poorer condition at birth (65), perinatal death (66), dyslexia (67), delayed speech development (68), and non-right handedness (69) (70) (71) (72)” – which as mentioned before is completely normal in many individuals, but may also indicate a disruption in brain development for some who were originally predisposed to right-handedness.
- One study “found brain hemorrhages in mouse pups exposed in the womb to pulsed ultrasound at doses similar to those used on human babies.” (13)
- “Other researchers found that a single ten-minute pulsed ultrasound exposure in pregnancy affected the locomotor and learning abilities of mouse offspring in adulthood, with a greater effect from longer exposure time.” (13)
- A study “involving newborn rats, who are at a similar stage of brain development to humans at four or five months in utero, suggested that pulsed ultrasound may damage the myelin that covers nerves (50), indicating that the nervous system may be particularly susceptible to damage from this technology.” (13)
- “Other experts in this area have expressed concern in relation to heating of the developing central nervous system, whose tissues are sensitive to damage by physical agents including heat. Barnett, a biomedical physicist, notes that heating of the fetal brain is more likely after the first trimester (three months), as the skull bone is more developed and can reflect and concentrate the ultrasound waves. (44)” (13)
Is it possible to minimize the risks of sonograms? ^
Yes. According to the ALARA (As Low As Reasonably Achievable) principle, the best way to minimize risk is to use the lowest setting and the shortest scan time possible to get the information needed.
Ultrasound equipment keeps track of two readings that make ALARA possible: the thermal index (TI) and mechanical index (MI). It is up to the sonographer to make sure the TI and MI stay within recommended ranges during ultrasound, but unfortunately many do not even know how to locate this information.
According to an article published at Contemporary OBGYN:
Unfortunately, the level of knowledge regarding ultrasound safety issues appears to be less than desirable. In a 2005 survey of attendees of European postgraduate obstetric ultrasound courses, only 22% and 11% of the participants could explain the TI and MI, respectively, and only 28% could locate this information on the ultrasound screen.33 A similar survey of American ultrasound operators conducted in 2007 revealed comparable results: 17.7% and 3.8% of the participants could describe the TI or MI, respectively, and 20.8% could locate this information on the display.” (emphasis mine)
If an ultrasound is planned, it might be wise to discuss in advance whether or not the sonographer has appropriate safety knowledge and enough experience to perform a thorough scan quickly.
The decision to have an ultrasound (or not) ^
. . . . is a very personal one. Although an ultrasound, or multiple ultrasounds, are often presented as an essential part of prenatal care, the American Pregnancy Association clearly states that:
Because ultrasound should only be used when medically indicated, many healthy pregnancies will not require an ultrasound.” (17)
Having said that, there is more to this decision than just one factor, and mama’s have an innate wisdom about these things that must be considered.
I wholeheartedly agree with what my friend Genevieve says The Mama Natural Week-by-Week Guide To Pregnancy & Childbirth regarding the 20-week anatomy scan:
If you’re trying to limit the number of ultrasounds you receive but still want one to check baby’s growth and development, however, this is the one to do. Keep in mind that there is a sweet spot in terms of when to undergo the procedure. Too early, and it’s possible that baby’s organs aren’t developed enough (or visible enough) to be properly evaluated, so the test may need to be redone in a few weeks. Too late, and it becomes hard to accurately measure baby’s growth. For these reasons, my midwife recommended that I postpone the ultrasound until Week 22; you’ll find that most healthcare providers have no issue with this.
As I wrote at the beginning of this article, after reviewing the research I chose to be selective about the use of ultrasound during my pregnancies, opting for one only if medically indicated. Your approach may be different, and I completely support that.
Did you have a prenatal ultrasound? ^
Why or why not?

Want to learn how to have an awesome birth without leaving your couch? ^
If you’re looking for an evidence-based, naturally-minded resource, I highly recommend the Mama Natural Birth Course and/or The Mama Natural Week-by-Week Guide to Pregnancy and Childbirth.
You’ll learn about:
- Delayed cord clamping, which boosts baby’s iron stores by 30% and improves fine motor skills and social development later in life.
- Skin-to-skin contact, which regulates baby’s body temperature and blood pressure, reduces stress hormones, and helps initiate early breastfeeding.
- Gentle cesarean, which can “seed” baby’s microbiome, eliminate fluids from baby’s lungs, while empowering the mama.
- The importance of eating during labor, and so much more.
Click here to check out the Mama Natural Birth Course, and here to check out The Mama Natural Week-by-Week Guide to Pregnancy and Childbirth.
Sources for this article:
1. Whitworth, M et. al. (2010) Ultrasound for fetal assessment in early pregnancy.
2. Bricker, L et. al. (2008) Routine ultrasound in late pregnancy (after 24 weeks gestation).
3. Alfirevic, C et. al. (2010) Fetal and umbilical Doppler ultrasound in normal pregnancy.
4. Bucher, H C et. al. (1993) Does routine ultrasound scanning improve outcome in pregnancy? Meta-analysis of various outcome measures.
5. Ultrasound Care. Dating and Viability.
6. Cohain, J et. al. (2012) Prenatal Ultrasound Does Not Improve Perinatal Outcomes.
7. Cooper, C (2013) Length of pregnancy can vary by up to five weeks, scientists discover.
8. Queen Mary University of London. The Quadruple Test.
9. Oyelese, Y et. al. (2009) Placenta previa: the evolving role of ultrasound.
10. Greene, G et. al. (2017) The Woman Who Knew Too Much, Revised Edition: Alice Steward and the Secrets of Radiation.
11. Richmond, C et. al. (2002) Alice Mary Stewart.
12. Heffernan, M (2012) Gentle Birth, Gentle Mothering: A Doctor’s Guide to Natural Childbirth and Gentle Early Parenting Choices
13. Buckley, S (2008) Gentle Birth, Gentle Mothering: A Doctor’s Guide to Natural Childbirth and Gentle Early Parenting Choices
14. Orenstein, B W (2011) The ALARA Principle and Sonography.
15. Siddique, J et. al. (2009) Trends in prenatal ultrasound use in the United States: 1995 to 2006.
16. Helliker, K (2015) Pregnant Women Get More Ultrasounds, Without Clear Medical Need.
17. American Pregnancy Association (2017) Ultrasound: Sonogram.
18. Debost-Legrand, Anne et. at. (20140 False positive morphologic diagnoses at the anomaly scan: marginal or real problem, a population-based cohort study.